
I prefer to start with the foot relaxed in natural plantarflexion with no dorsiflexion (DF) initially and then advance to full DF as tolerated. Keep in mind that maximum dural tension occurs with full DF at the bottom when the head/trunk is also flexed. Perform 1-2 sets of 10-15 reps daily.
 |  |
Many people between the ages of 30 and 55 deal with degenerative disc disease and mechanical back pain. Unquestionably, the sitting we do is hurting our spines. Over time, the lumbar disc may slowly shift and creep backward exerting a growing pressure on the sciatic nerve roots. This may even lead to intermittent or consistent local and/or referred pain. Some will even experience numbness and tingling along the posterior and/or lateral side of one leg).
If this goes on long enough, the dural sheath that encases the sciatic nerve becomes inflamed, and the sciatic nerve may become adhered and lose its natural mobility. I frequently see this manifested in what appears to be hamstring tightness on one side compared to the other. In many cases, a hamstring stretch does not reproduce referred pain but simply elicits reports of "increased tension or tightness" from the client.
In my experience, clients often mistake chronic and subtle nerve issues with hamstring strains or piriformis syndrome. Restoring nerve mobility is important for long term recovery and health (think myofascial chains here). Some research even suggests neural tightness may contribute to HS strains. In clients who seem to have asymmetrical HS flexibility with a history of prior low back pain or HS strains, this should be part of their routine mobility training.
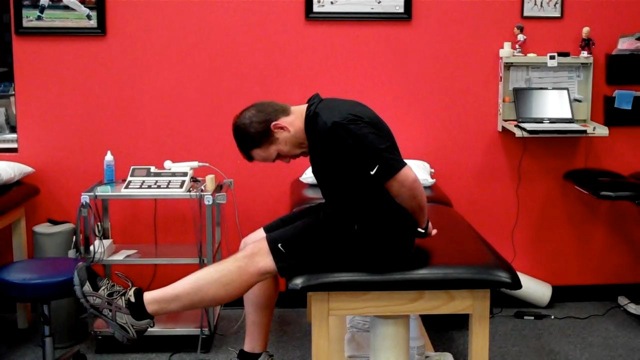 | 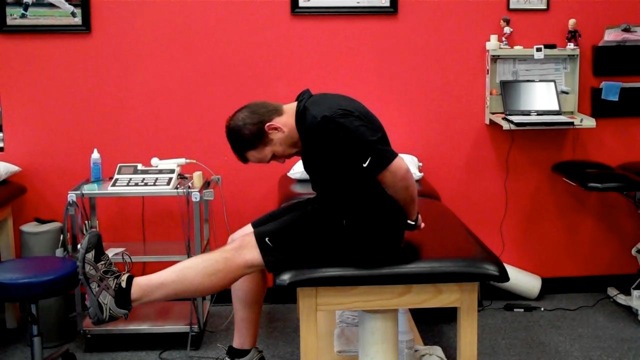 |
Modification:
If this position is uncomfortable or contraindicated for any reason, clients may attempt a nerve gliding technique in supine. They simply flex the involved hip and knee to 90 degrees (the other knee is flexed to 90 degrees with the foot flat on the floor). Grasping the posterior thigh, the client slowly extends the knee (hip remains at 90), pauses at the top for 1-2 seconds, and then slowly returns to 90 degrees of knee flexion. Again, I start with no DF and then progress to maximal DF.
Precautions/Contraindications:
In clients with acute low back pain or peripheral symptoms, you should refer them to a medical provider immediately for further evaluation prior to prescribing this exercise to ensure their back is stable and to avoid exacerbating any existing condition they may have.
Brian Schiff, PT, OCS, CSCS, is a licensed physical therapist, respected author and fitness professional. Currently, he serves as the supervisor at the Athletic Performance Center in Raleigh, NC. Brian presents nationally at several professional conferences and seminars on injury prevention, rehab and sport-specific training. For more cutting edge training information, subscribe to his monthly Training & Sports Medicine Update at www.BrianSchiff.com.
















